A basic journalistic precept says that a journalist should be objective and unbiased in an interview. But I'm going to make an exception this time. This will be the first interview in which I will be, I admit, biased.
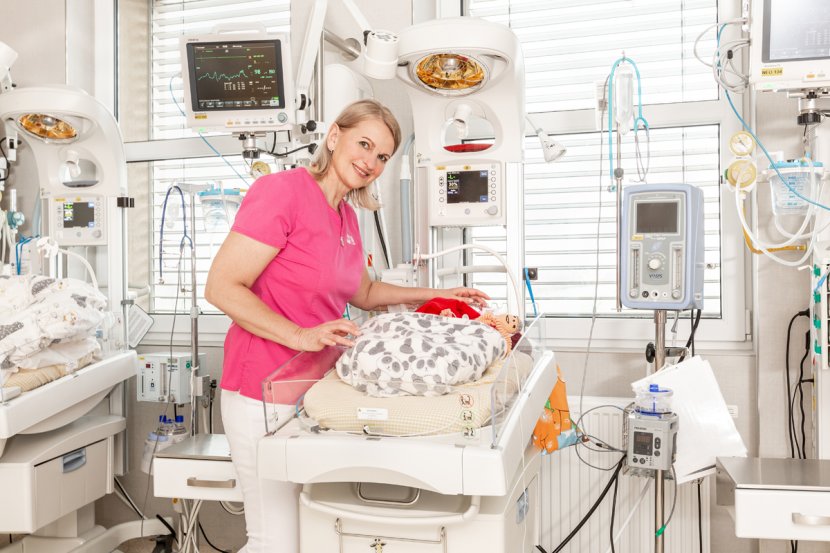
In mid-December, our son was born at the Hořovice Hospital. It was the most beautiful Christmas present you can imagine, except that we unwrapped it a little early. Almost two months earlier, because he was born at the end of the 32nd week of pregnancy. We spent the next month, Christmas and New Year's Eve in the neonatology ward, and became parents in a place where no one wants to be a parent. A place where strong men cry, where the most impressive stories are written and where miracles happen every day with the help of angels, nurses and doctors. To this day, I still don't know if Milena Dokoupilova, the head of neonatology, is more of an angel or a doctor, but she probably has a piece of each. From the first moment she led me to the incubator after the birth and showed me the two-kilogram human I wasn't supposed to properly meet until eight weeks later, she never for a moment made me doubt that maybe he wouldn't make it.
She has been caring for premature, technically speaking immature babies for almost three decades. She started in the Prague maternity hospital U Apolináře and for the last 10 years she has continued her work in the hospital in Hořovice, which has become one of the most popular maternity hospitals in the region thanks to her.
Hořovice is one of the top 25 centres in the Czech Republic that are able to take care of premature babies (before 37 weeks of pregnancy), specifically here they take care of newborns from the 32nd week of pregnancy, in some cases even from the 30th week. More than 1 700 babies are born here every year, of which around 250 need intensive care.
Watching every day with your own eyes what today's medicine combined with the experience and skills of Milena Dokoupilova's team can do with children who would have no chance of survival without them is an experience no one wants, but when you get to experience it, you are glad it is here. Forget about the cold and sad hospital environment - Dokoupilová has managed to build a pleasant place in Hořovice, where the birthing boxes resemble cosy hotel rooms, where the rooms for mothers look like home and where both parents are actively involved in the care of defenceless babies from the very first moment, which is still unusual in all neonatal intensive care units. "The biggest miracle for me is when the baby goes home. That's probably when I get more emotional than when they are born. Because at the beginning, my mind is racing with what we have to do, my thoughts are racing and there is no time to be moved. But when the baby goes home, you think: Yeah, that was good," Dokoupilová smiles.
Every baby has a mother who also needs care. Not medical, but psychological.
Can you count how many of these children have passed through your hands over the years?
You can't really count, because there is always a whole team involved in caring for children. Some of the kids you take care of directly, some of the kids you take care of in services. But I'll give it a shot. When I started at Apollinaris, there were about three thousand babies a year, and when I left, it was already five thousand. Of those, about 300 babies a year needed the most intensive care. I spent 18 years there. That's about five or six thousand babies. I've been in Hořovice for 10 years, over two thousand children needed our intensive care unit. So I'm sure it's thousands.
Out of those thousands of stories over almost 30 years, does one in particular stick out to you?
I wouldn't know which one to start with. I wonder which one was the most powerful.
Try to pick one.
You always remember the biggest screw-ups the most. And one of the toughest patients, ironically, was a premature boy who was in critical condition for four days, on the verge of surviving. The worst thing for a doctor in that situation is not to have good news for the parents and to have to keep telling them it's bad. To keep his mom from completely collapsing, I was trying to think of something to hold her up. And so we started playing a game together of calling the little boy a bastard. We agreed that one day when she came over and I called her a brat, it would be a turn for the better. It may sound harsh, but it worked. The boy eventually became a brat. Today he's 18 years old and it's all worked out well.
What happened then?
When a baby stops thriving in the mother's womb and is oxygen-deprived, the baby starts to pass smolka, or stool, in which case the baby tends to start struggling to breathe prematurely. That's what happened in this case. Even before the birth, the boy started inhaling amniotic fluid that had pitch in it, which clogged his lungs, which was a big problem. After the birth he was in a critical condition, it was either or. The next four days were really hard, where we alternated day and night with him. It was even harder for the parents, who we couldn't say anything positive to for four days.
They say birth is a miracle, but you are often at births where babies are born when they shouldn't be. Is it still a miracle for you then, or is it more about fear?
I'd say I'm more about anticipation. You always want the baby to be born in the best possible condition, because the beginning is so important. But you also know that you can't usually control it too much. That's why discussions between the obstetrician and the neonatologist are so necessary, where we address whether the baby is still fine in the mother's belly or would be better off outside.
Is it usual to prepare for premature birth in advance?
We usually can't prepare for it. I would say only 30-40 percent of preterm births happen after moms have been lying here for a few days, most often with amniotic fluid draining or high blood pressure. But most births of immature babies happen within 24 hours of moms being admitted to the delivery room. The most difficult times are when the mom comes in for a routine check-up and has no problems. And suddenly she learns that we have to terminate the pregnancy because the baby is no longer doing well in the tummy.
What do you care about when you know you're going to have a premature birth?
I care about the week of pregnancy because it has to do with the likelihood of what will happen to the baby after birth. Then I ask about the mum's medical history, her associated illnesses, whether she is taking any medication. Information about the administration of corticosteroids to support lung maturity is also important. And last but not least, I want to know how the baby will be born.
But most of all, after birth, it's about the lungs and how mature they are, right?
Yes. But that goes for premature babies too. It's technically called cardiopulmonary stabilization. The heart has to get the blood flowing as it should. Some blood vessels have to open, some have to close. And most importantly, after birth, the blood has to start oxygenating in the lungs. All this happens in the first few breaths of a newborn. It's the same for all babies, but for premature babies there may be an added factor of lung immaturity.
How does this manifest itself?
When a baby is born, his lungs are full of water, he has to exert tremendous pressure to push the water out and get air into his lungs. If the baby's breathing activity is not satisfactory after birth, we sometimes have to help him artificially, by pressurising him with a ventilator. A greater problem can occur in immature lungs when the lung chutes are unstable and may collapse. The presence of surfactant is needed to keep them well developed after expiration. This is a surfactant that is physiologically produced by a particular type of lung cell.
And the premature baby hasn't had time to develop this...
Surfactant starts to form in small amounts from the 24th week of pregnancy, gradually increases, but is not fully formed until around the 36th week of pregnancy. Today we can provoke the lung cells to start producing surfactant earlier and faster by administering corticosteroids before birth. Alternatively, we can get it into the lungs artificially after birth. Today, surfactant is produced industrially thanks to US President Kennedy, whose premature son died 39 hours after birth in 1963 because of lung immaturity. In this country, surfactant was first administered artificially into the lungs in the late 1980s; until then, babies born in the 34th to 36th week of pregnancy died of lung failure.
So what do you prepare parents of premature babies for?
I always try to tell mothers only what is highly likely to concern them, so as not to overwhelm them with information. So maybe your lady knew that your baby may need controlled pulmonary ventilation because at 32 weeks there is still a risk. I try not to give too much negative information, but on the other hand, you need to pour yourself a glass of wine. Moms also need to hear that their baby will look completely normal, just a little smaller. They're so scared that he'll miss something. They need to know what's likely to happen after birth. For example, babies who are born at 34 to 36 weeks are often very dexterous at the beginning, they improve quickly in the first few days, they learn to suck. But 80-90 percent of them gradually get tired, and at the end of the first week there is usually a period when they are suddenly sleepy, tired, and what they have learned they suddenly can't do. And if we don't prepare moms for that ahead of time, they start to break down.
What's the most common question you get?
When's the baby coming home. You can never tell exactly, but most babies go home by their scheduled due date, often sooner, most often around 36 weeks gestation. They need to be stable in breathing, be able to eat on their own and thrive on weight. Sometimes it's a big struggle and a never-ending story for everyone involved.
If the baby is going to be born prematurely, is there a "best" time for it to happen?
No, that's just old wives' tales. It belongs to the myths surrounding childbirth. A simple mathematical equation works that every extra week or day in the mother's belly is simply better.
Yet they say it's better to have a baby in the seventh month rather than the eighth.
That's just one of those superstitions. At seven months, everyone expects a problem, so they're prepared for it. But the tricky thing about the eighth month is that 95 per cent of babies are completely fine, it's just that the few per cent that are then really worth it. Unfortunately, those babies can die. Ironically, historically, these babies have died more than much more immature babies, so I guess that's where these superstitions come from.
Speaking of your care, I watched it up close for a month and I confess that the sight of a baby fighting for its life moved me every time. Are you moved after all these years?
Yeah. I still do. I'm still worried about those babies because I've seen and experienced so much. Premature babies are less likely to have anything happen. That's why I'm paradoxically even more worried about these babies - you never know what they're gonna do to you. I confess I'm a terrible pedant and a stickler. I can't stand, for example, just a folded, wrinkled blanket under a baby because I know that if he doesn't have good blood flow in his skin, he'll easily get a blister. Sometimes I annoy my nurses with this, but most of them have gotten used to me and understand that I don't want to bother them, that it's just my experience that can help prevent complications. Nurses are absolutely crucial to our field. They are the ones who make all the difference. How they position the baby, how they keep the airway clear, how accurately they administer the medication on multiple dilutions, how they teach the mom to manipulate the baby. Not many girls want to do that because they're so scared. That's why I'm very proud of my team of nurses and doctors and I respect them so much. But without my head nurse, Kamila Prádová, I would be like without an arm, or rather without hands.
What's the best part of the job for you?
It's when the baby goes home. I guess I get more emotional when babies go home than when they're born. In the beginning, it's more about what we have to do, what we can't forget. The thoughts are swirling, that's just the way it is. But when the baby comes home, you think: Yeah, that was good.
How did you get into neonatology in the first place?
I never wanted to go into medicine, but my mum pushed me into it in my last year of high school. While studying, I managed to get married, have a child and move from Olomouc to Prague. When I graduated in 1993, it was a problem to find a job as a doctor. I didn't have any big ideas, just that I would rather work with children. I went around to all possible hospitals and bothered for so long until I got to the selection process at Apolinar for the neonatal ward. I thought "newborns, I don't know", but I gave it a try. I was selected and I quickly found it really interesting, and soon the field became my heart's desire.
And from the beginning you were involved with premature babies?
Like any young second year student, I had to learn about healthy newborns first. But I stayed with neonates, I only did pediatrics as part of my pre-service internship. Then I started to focus on immature babies. I was very interested in different techniques of ventilatory support; in the 90s we made some of the devices almost on our knees. When I got an offer to work in Hořovice in 2011, I was afraid that I would miss the smallest children. But working with the bigger kids, over a kilo, is interesting too. So I don't miss them. However, several of the under-pounders were unintentionally born here. And to keep up to date with the care of the little ones, I sometimes go to Podolia to serve.
Neonatology brings many beautiful moments, but also tragic ones when a newborn dies. You must have experienced many such sad stories.
Yes, but less here than at Apollinaris, because in neonatology it is mostly related to the degree of immaturity, we don't have the most risky babies here. The death of a child is always harder to accept than that of an adult, it is the beginning of life. Everybody thinks it's hard just to receive the information about death, but it's just as hard to communicate it. One must have a certain amount of empathy, which is either a gift or acquired with experience. Unfortunately, there will never be a time when not a single newborn dies. In the 10 years I have been here, we have delivered several babies, mostly with serious congenital developmental defects that were intractable. It's always a sad moment, that's when you're there for the parents, you're not dealing with yourself. The most important thing is to communicate, to call everything by its real name, to help the parents to live this moment. It's similar with critically ill children.
Do you have an example?
We had a baby delivered here, 70th hour of life, was due to be discharged home the morning after rounds. I was past my bedtime and getting ready to go home. I forgot something else and the ward, so I came back. Suddenly the door burst open, the young doctor was carrying the baby in the cot from mummy's room and just said to me: Come quickly with me. I pulled back the covers, the baby looked terrible, bulging eyes, dark spots on the skin. We immediately started CPR and called the neonatal transfer service in Prague. It was clear that the baby was going to have some serious problem, we just didn't know what it was yet. All lab blood values were basically incompatible with life. When he left, we didn't know if he would survive.
What happened?
Eventually, it was a critical heart defect, the baby was operated on. He's three years old today and he's fine. But why am I telling this story - communication with the parents. Imagine the situation. Mommy all made up, packed up and ready to go home. Without knowing anything was wrong. Suddenly the doctor comes in and tells her the baby doesn't look good at all. Then you gradually explain that her baby is almost clinically dead. You have to communicate with her, but at the same time resuscitate her because time is flying by. And it's an absolutely horrible situation. The mother's hanging on to you with her eyes, she doesn't understand, because she had a perfectly healthy baby just a moment ago. That's when I ended up seeing a psychologist for the first time in my life, because I couldn't stand it. I'm still friends with a lot of those parents to this day. I guess sometimes I let those kids into my life too much, but that's just the way I am. I don't think I'll be any different. Just the other day, I got an email out of the blue from a 21-year-old I used to take care of, saying she wanted to thank me for everything, that she was going to college. She weighed 900 grams and was born at 26 weeks gestation. She even sent me a picture of me holding her as a baby when she went home. You don't know whether to laugh or cry. You just find it all makes sense.
What is your success rate with premature babies in Hořovice?
To put it simply, the babies we care for here, babies over 30 weeks gestation, have no reason to die. But of course they can die too, from an infection or from some congenital developmental defect. That's where caring for moderately immature babies is nice, because the sad moments are minimal.
What is the minimum threshold for saving babies today?
In the Czech Republic, the limit is set by law at 24 weeks of pregnancy. Each state has its own rules. In Japan, for example, babies are taken care of from the 22nd week of pregnancy, and in Denmark from the 25th week. So the Czech Republic is somewhere in the middle. In these lowest weeks, babies usually weigh around 500 grams. The smallest baby in the world who was born and survived was in the United States and was 280 grams. In the Czech Republic, I think the record is 310 grams. The postnatal adaptation is similar, but you can run into technical problems of how to secure such a little person for breathing, infusion. You have to insert tubing into the tiny body, which has a certain diameter. That takes a lot of skill. That's why I'm convinced that you can't push the boundary much lower. But who knows?
How big is the risk of permanent consequences for babies born this early?
It's generally put at around 20% for those who survive. But it very much depends on what diagnoses the child goes on to get before going home. The fewer there are, the better the chance of a normal life. Brain haemorrhage, repeated infections, chronic lung disease, retinal disease, these are all diagnoses that can affect his development.
Hořovice is one of the top 25 centres in the Czech Republic that can take care of premature babies.
Knowing that the child has been ventilated for two months and needs further pharmacological treatment, heprobablywon't be a top athlete, but he can have a normal life, maybe more frequent respiratory infections in the first years. But if he has had a severe brain hemorrhage, the likelihood that it will negatively affect his development is great. On the other hand, the human brain is astonishingly plastic, so much so that I sometimes wonder what these children can endure and handle. Anyway, when the probability of a problem is great, it is necessary to talk to parents about all the possibilities, there is no point in being silent. I think I can be very hopeful. You can't do this business without hope and optimism, but that hope must never be false. We're talking about a field where you're constantly on the edge of ethics and morality.
Have you ever had parents not want you to save a premature baby because they were afraid of the permanent consequences?
Yes, I have. But fortunately, the law makes this a little easier. It says that if a live baby is born at the completed 24th week of pregnancy, I have to provide medical care. I can't do otherwise as a doctor. But I can discuss with the parents before the birth whether to resuscitate a baby on the verge of viability. Studies show that when such an immature baby needs to be resuscitated, its prognosis worsens significantly. It is terribly individual, so parents must be listened to and told of all the risks, but their voice must be advisory only. I'm a doctor, and I have to take the responsibility in the end. A doctor learns to work with that decision-making feeling over time, but a parent doesn't.
This brings us to the distinctive feature of Gorovice neonatology - from the very first moment you involve the babies and their mothers much more than usual in their care. Why?
It has always been important for me not only to care for babies, but also for their parents. Every baby has a mother who also needs care, not medical but often more psychological. I've always had it this way, nobody led me to it, but somehow it came out. Even when I started at Apollinaris, I was always sitting on the floor by the incubators and talking to mothers who were cloning their miniature babies. We talked not only about their babies, but about life in a normal way. I try to get the mothers to touch the baby as soon as possible, to stop being afraid, to start taking the baby's temperature, to start changing the baby. We don't leave out the dads either, even though they sometimes discuss it with us. I've never been the scientific kind of doctor, so I tend to write books for moms because I think they appreciate it and I think it's needed. The current trend of not separating mother and immature child is getting closer and closer to my lifelong belief.
The fact is, I didn't even feel like I was in a hospital. In the ICU, the fathers of the children can join them without restriction and, if there is capacity, they can spend the night here. Does that put more demands on hygiene?
It doesn't. The father is part of the family and belongs to the child as much as the mother. This is doubly true for premature births, he is often the most important support for the mother. When I came to Hořovice and told the institutional hygienist what I intended to build here, she was frankly horrified. She was most afraid of neonatal infections. An immature newborn was always a terror. I told her: One day there will be a large intensive care unit for newborns and their parents to care for them. I still remember the horror in her eyes, even though it was 10 years ago. We have strict rules on the ward, perhaps stricter than would be appropriate for such immature babies, but it pays off. We have almost no serious nosocomial infections (infections that children acquire while on the ward). Finally, even our hygienist acknowledged that it can work and invited me to give a lecture to the field hygienists of the Central Bohemia Region about the hygiene regime in the neonatal ward. Changes are made easily not because of reluctance, but because of fear and apprehension.
Your ward does not look standard, it feels more like a cosy hotel than a hospital. Whose idea was it?
Mine. It was a great dream come true, but it was only possible thanks to the owner who supported me in my idea. He likes newborns very much himself. But I must admit that when I came to Hořovice, I had no idea how far we would go. We started in the sixth-grade ward, in the observation box for physiological newborns with four beds. Gradually we grew until one day the owner came up with a plan for an extension for a completely new intensive care unit. I'm quite the technical type, I normally keep a screwdriver handy. I just had the load-bearing walls marked on the project and then I just painted and painted, for almost a year. There were many variations, the current one is 52. I had a lot of fun logically figuring out what outlet, switch, wall, door would go where. Newborn needs are specific, a lot of things were specially made. The architect would then translate my painting into projects. And once the layout was done, it was the design's turn.
But you didn't want it to look like a hospital.
Exactly. The designer gave me a very simple brief. I think she exceeded my expectations. There are some things you can't change - a baby is going to be born, it's going to have some problems, and mom is going to have to be here with it. But you can change that, she'll feel a little better if it's nice, cozy around her. And that's what's been done.
Pavel Kalouš, Néa I Spring 2021 I No. 8