Therefore, the staff talks mostly with the parents of these children, so it is not only medical help, but also psychological help. This department at the Hořovice Hospital in Beroun is officially called the Department of Long-term and Intensive Nursing Care for Children (DIOP), not the Palliative Care Department, as its head, Mahulena Exnerová, always emphasises. Palliative care is only one part of the complex care for children with such illnesses. Although there are children with very serious and incurable diseases, most of them survive for many months or years. Twenty children have passed through this special ward in the two years it has been open. Five have died.
"It must be remembered that paediatric palliative care patients are different from adult ones. While 80 per cent of adults are cancer patients at an advanced stage of the disease, the vast majority of children are non-cancer patients with a very broad spectrum of diagnoses. These include various congenital, genetically based syndromes, inborn errors of metabolism or neurodegenerative diseases," says Exner. Similarly, in Hořovice they treat children with very rare diseases, of which there are few in the whole country, after severe injuries or with severe forms of epilepsy. "The time a patient can live with these diseases is longer than for severe cancer patients, and so the treatment time for these patients is longer," Exnerová explains.
These children have what is known as an uncertain prognosis, meaning they may die just days after birth, or they may also live into adolescence or young adulthood. There are also diseases where everything seems normal at first, the child grows and thrives like all his peers, but gradually as he gets older, it becomes clear that his condition is deteriorating, and he dies within a few years. "It is therefore extremely difficult to make any kind of prognosis for such sick children, because no one can accurately determine the life expectancy of these diseases," says Exner. Even two children who have the same disease may not have the same course. It depends, for example, on whether or not severe complications develop.
Sick children live longer
A positive example of a child who overcame a negative prognosis is a 17-year-old boy who, after a serious motorbike accident, ended up in the local ward in a so-called apalic state (vegetative state with a special type of disturbance of consciousness, the patient is lying down with his eyes open, ed.).
For several months he did not move or communicate much and the doctors did not give much chance that his condition would improve. "But then a literal miracle happened. The boy began to respond, communicate, exercise with us and his parents, and his condition improved so much that after a year we released him to home care. The consequences will remain, he will never be like a healthy teenager, but he can live a very good life," Exner assumes.
In addition to the six long-term intensive care beds, Hořovice also has a separate ward with 13 beds for children who need ventilator support, as this may be necessary for some diagnoses and conditions.
With the development of modern medicine, the survival of children with serious, life-limiting illnesses is being extended. An example is cystic fibrosis, which is still a very severe disease that, among other things, fundamentally affects the airways. Over the last 30 years, the survival time of children with cystic fibrosis has increased very significantly. "Back when I was still studying, children with the more severe course of the disease tended to live to about adolescence. As prevention, inhalation or lung transplantation options have developed, survival for these patients has extended well into young adulthood. And so it is with many other diseases, such as cerebral palsy. We are simply improving the medical options and extending the survival of our pediatric patients," says Exner, herself the mother of a 16-year-old daughter.
According to Mahulena Exnerová, palliative care in the Czech Republic has moved forward very significantly in the last 10 years. While it used to be the concern of fragmented groups of doctors and non-medical professionals, today it is becoming a well-established and respected branch of medicine. In 2014, the first conference focused on pediatric palliative care was held in the country. In 2015, a working group on paediatric palliative care was established and two years later paediatric palliative care began to exist as a separate section within the Czech Society of Palliative Medicine.
Since then, the development of this care has been moving forward rapidly in many aspects. "It has been a topic that has been discussed for the last five years, and I think it is important that it is moving forward so strongly," praises Exner.
Life changes for parents and siblings
A big topic in paediatric palliative care is the parents of young patients, who can live and care for their offspring on the ward or visit them without restrictions. Often the possibility of communication with parents is even more intensive than with patients. That is why the team of professionals here includes not only doctors, nurses and physiotherapists, but also a social worker, psychologist or chaplain. They are an important practical and psychological support for parents.
"It is particularly difficult when a family suddenly has to come to terms with the fact that their offspring has a serious diagnosis. Some children are born with such a diagnosis, but for some the diagnosis appears suddenly, for example as brain damage after an accident, or if the child has undergone prolonged resuscitation. Then the brain has not been oxygenated and suddenly a healthy child is severely neurologically impaired with little prospect of improvement," Exner notes. In such a case, the family needs time not only for their offspring's condition to stabilize, but also for the parents to learn how to care for their child and to adjust, for example, housing and all other activities accordingly. In all likelihood, one parent will have to leave their day job, stay at home and care for the child, which is usually 24 hours a day, seven days a week.
"It's always a huge change in the whole family, not just for the caring parents, but for the siblings as well. It's something that takes time. The family has to be equipped with the necessary tools and trained in caregiving. Sometimes it feels like an intensive care unit in the apartment of these families, with a special bed and all the equipment," Exner says. The team of doctors here supports the family as a whole, and in addition to the necessary help of a clinical psychologist, the support of a social worker is also very important. For it is essential for the family to secure all possible allowances and to procure other follow-up services in the field, such as home care, transport, education and so on. The chaplain, in turn, helps to care for the spiritual needs of the parents.
It is beneficial for the family to have somewhere to turn, someone they can call for advice. Simply knowing that they are not on their own and that someone is there to guide them through this difficult situation. "We also always try to create a realistic care plan with the family. Sensitive but very open communication is important. This means talking truthfully about the illness, what the prospects are and what can happen during the course of the illness, what we need to prepare for and what we can manage together," says Exner.
She talks to the parents of patients about what is important to them, what they would like for their child and what they consider to be a good quality of life for their offspring. Accordingly, they then create a care plan together, which must have as realistic an outline as possible and which includes a plan B. That is, preparation for when complications arise. "In palliative care, we always prepare for the worst and hope for the best. We really go through with the parents the possibility that maybe a serious infectious complication may come, what it will look like and what they would want to do in that situation. Would they want to be in the hospital with their child or would they want to be at home," says Exner. Such conversations are not easy, they are repetitive and often last for many hours. But they are essential to setting up the right treatment.
A project to establish palliative care has been launched
Exnerová greatly appreciates the fact that since 2018, insurance companies have been reimbursing the care of mobile hospices, which go directly to the homes of the seriously ill to care for them, and also that palliative care is now becoming a full-fledged medical specialty in Czech hospitals. For example, there is now a European Union pilot project being implemented by the Ministry of Health in cooperation with the Czech Society of Palliative Medicine and co-financed by the EU. The implementation team of this project is composed of leading experts in palliative care and representatives of the Ministry of Health. They meet once a month to discuss the key activities of the project.
As part of this, seven consortium palliative care teams are piloting this type of care in six selected hospitals. One of the supported teams is the only purely paediatric team at Motol Hospital. As a result of this project, there is now a unified consensus position of professional societies on palliative care. The expected outcome should help to establish a stable, long-term functioning and financing of hospital palliative care in the Czech Republic.
HOSPITAL HOŘOVICE
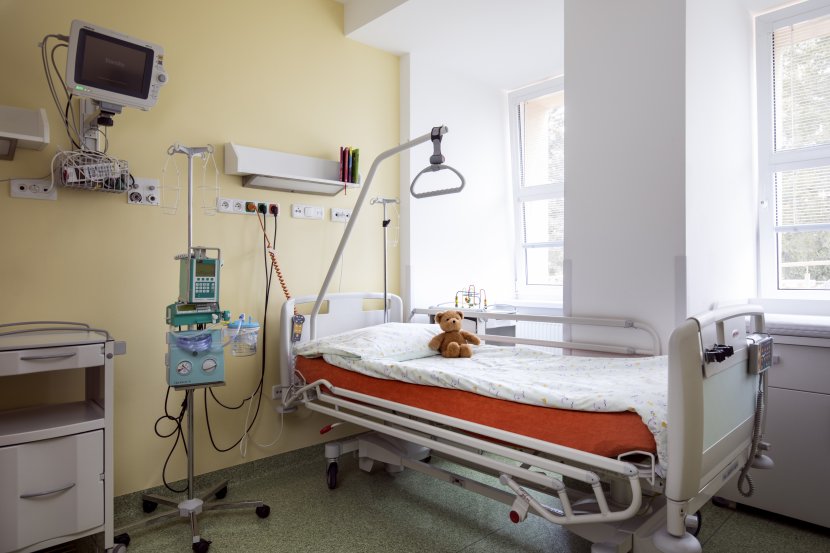
The department of long-term and intensive nursing care for children was opened in September 2018. This ward has fully equipped beds in separate rooms where parents can stay permanently. The ward accommodates children with serious, life-limiting illnesses. The care covers not only physical health symptoms, but also psychological, social and spiritual aspects. Mahulena Exnerová (on the left in the bottom photo), who previously worked for example at the Motol Hospital in Prague, is the head nurse of the children's ward Jitka Lacinová.
Source.