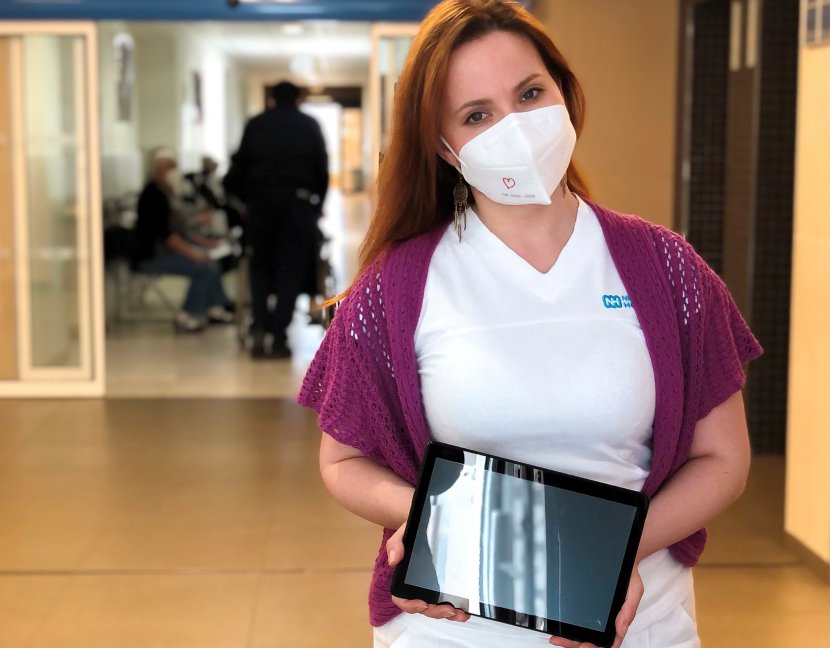
Why was the service of video calls between patients and relatives introduced?
As a hospital, we strive to care for people with all their needs. The situation we have been in for a long time is challenging in itself for everyone. The great restriction of visits, the necessity of which is undeniable, is very psychologically challenging not only for the patients and their families, but also for us, the staff. In the autumn, as part of the hospital's palliative care team, we began to consider ways to support patients, families and staff through this difficult time. One idea was to give patients contact with their loved ones. It didn't take long from idea to implementation, and the management was very receptive to the idea. Tablets were purchased for each ward, and the necessary applications were installed to enable video calls to take place. From the very first moment, it was obvious how useful this service is, and in the more than four months that we have been facilitating it, I have only become more convinced of this idea.
What is the interest in this service?
To date we have connected a total of approximately 120 calls for a total of 46 families. We try to tailor the frequency, call length and time to the needs of patients and families as much as possible. Sometimes all it takes is one short connection, the reassurance that we can see each other, hear each other, that we "know" about each other. Other times it is a very intensive communication, multiple connections over a longer period of time, as hospitalizations can vary in length. It is also important to get the word out that we offer this service in hospital and that they can request it at any time during their hospital stay. I think that for the number of hospitalised patients, the number of calls could be higher. But I am still pleased with the interest so far. All the families have been very grateful for the opportunity to connect.
Can relatives also contact you or does the request have to come from the patient?
Anyone can contact me. Patient, family, doctor, nurses, paramedics... It doesn't have to be a specific request. It can be a suggestion such as the patient is mentally distressed, sad, remembering his family. If a doctor or other worker who is in daily contact with the patient gives me this information, I can work with it further, visit the patient, call the family and offer them a video call. And it's not only these calls, but also, for example, someone from the family sent me photographs that I could then look at together with the patient or perhaps read a letter.
How does this work in practice?
In practice, it looks like a family who is interested in hearing and seeing their loved one calls me or a doctor calls me and says that the patient would like to see the family. Based on this, I arrange the specific details with the family - the date of the connection, the approximate time, and also the app we will use for the connection (most often we use whatsapp, but we have also connected via messenger or viber). If we already have everything we need arranged, nothing prevents us from making the call. At the given hour, I visit the patient in the room and we connect the call. I stay with the connection for assistance, sometimes help is needed with communication, etc. The frequency of the connection depends on the agreement. Sometimes we connect once, other times it is 3 times a week for several weeks. It depends on the specific situation and the family, we try our best to accommodate everyone who is interested.
More often than not, I connect older patients who either don't have a phone at all or don't have a modern device that allows them to video call. Even a patient with impaired consciousness, a patient who does not communicate verbally or a patient who is confused is not a barrier to connection. Here again, the connection can be very helpful as it can be supportive and beneficial to the patient's psychological well-being to hear a familiar voice, but also to the family as reassurance that their loved one is doing well. Because visits are severely limited on all wards, we connect patients with covid but also with other diagnoses.
If the situation is urgent or if the connection cannot be made within working hours (Mon-Fri, 8am-4.30pm), it is no problem at all to arrange a later time or weekend.
Will you continue this "service" after the end of the measure, when visits are possible?
I have already thought about this idea because we have been connecting families from the other side of the country or families abroad (Germany, Belgium, Spain). I think this is one of the positives that this time has brought us and has shown how beneficial this way of communication can be. I can imagine that video call facilitation will be a standard service in cases where a personal visit is not possible for some reason (distance, health limitations or other).
Have you ever had any interesting situations in this context?
Call mediation brings many different experiences. From funny, touching, even very sad, depending on the specific medical and family situation.
When I connect families more often, I become part of their story. Through conversations we experience different emotions, from joy, relief, love, to sadness, fear or hopelessness. To see a couple send kisses and profess their love to each other after fifty years of marriage, to see little grandchildren with their carefree smiles greeting their grandmother or grandfather, to see perhaps half the family gather around the screen to greet a loved one and at least in this way give them strength and hope. These are very powerful and important moments.
Sometimes these situations are very challenging for everyone because the stories do not always have a happy ending, but even in these moments we try to be there for our patients and their loved ones.
| If you have a loved one in hospital and would be interested in facilitating contact with them, please do not hesitate to contact me. The service is free of charge. hylova@nemocnice-horovice.cz, tel. 702 204 703. |