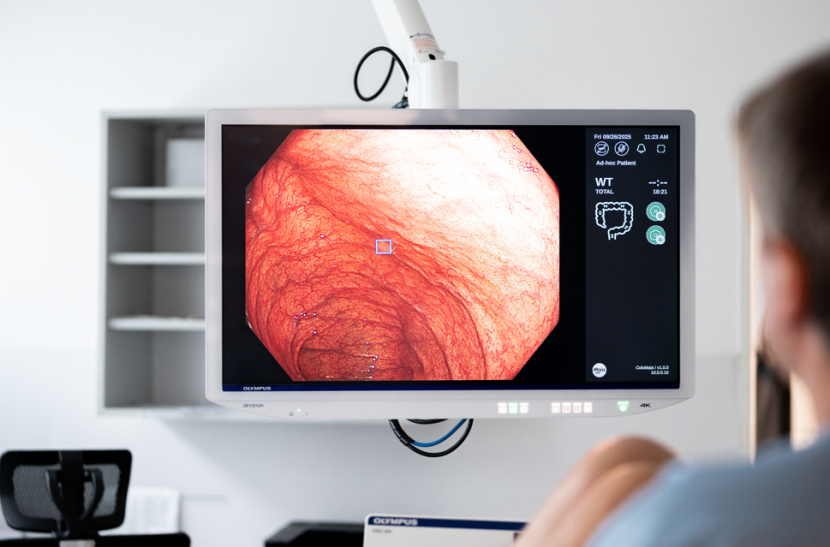
What is Maia and how does it work during a colonoscopy?
Maia is our new "second pair of eyes" based on artificial intelligence. It monitors the endoscope image in real time and alerts us to areas that may correspond to polyps or other suspicious lesions. A subtle highlight or box appears on the monitor and the system emits a short audio signal. However, the final decision on exactly what we see and how to proceed is always up to the doctor. Technically speaking, this is computer-assisted detection (CADe) and in the advanced mode the system can also offer an indicative characterisation of the finding (CADx).
What are the advantages of this system for the patient compared to traditional methods?
First of all, it increases the chance of detecting small or flat lesions that might be missed during a conventional endoscopic examination. Large studies show that AI increases the detection of adenomas by several percentage points. In practice, this means fewer missed polyps and a lower risk of so-called interval tumours between colonoscopies. At the same time, Maia helps us standardize quality across endoscopists.
How does Maia help you physicians?
It highlights subtle changes in the colour, texture and margins of the mucosa as we pass the endoscope through the bowel. In practice, this reduces the risk of 'blind spots' - for example, when we focus on navigation, suction or rinsing, the system keeps an eye on the image in the meantime. In some situations, it will also give us an indicative estimate of the type of polyp, which can support decisions about the optimal removal strategy.
Can Maia find all kinds of problems?
No system can replace the experience of an endoscopist and detect what is not visible on the camera. Maia most often detects adenomatous and other types of polyps. It performs less well when there is insufficient bowel cleansing, rapid endoscope movement, the presence of foam or active bleeding. Diseases without visible changes, such as microscopic colitis, it cannot detect. It is a great helper, not a substitute for a doctor.
Does the doctor have to undergo special training?
Yes, but it's short and practical. We trained the whole team in using the system and interpreting the alerts before deployment. The training took dozens of minutes and included coordination with the nurses. Formal certification is usually not required. The important thing is to approach the system sensibly, continuously evaluate its benefits and be able to work with false positives.
Is this examination covered by health insurance?
Yes. Colonoscopy is covered by public health insurance in the Czech Republic. Maia is part of the technological equipment of our department and the patient does not pay anything.
What determines whether to use the system during an examination?
The quality of bowel preparation, the indication for the examination and the professional judgement of the endoscopist determine whether the system is used during a particular examination. In urgent situations or very poor cleansing, the benefit of AI is reduced and therefore the system does not need to be switched on.
How do you see the future of AI in gastroenterology?
Very promising. We will soon move from detection alone to more accurate characterization of lesions, automatic measurement of their size and recommendation of the optimal course of action. AI has great potential in capsule endoscopy, where it can significantly reduce reading time and increase detection of bleeding or angiodysplasia. We also expect better mapping of foci of dysplasia in inflammatory bowel disease and in the oesophagus, and wider support for targeted (chromo)endoscopy. Integration with quality control tools and smart documentation will also be part of the future. And above all, AI should remain a safe and auditable "co-pilot". The final clinical decision will always be in the hands of the physician - and that's how it should be.